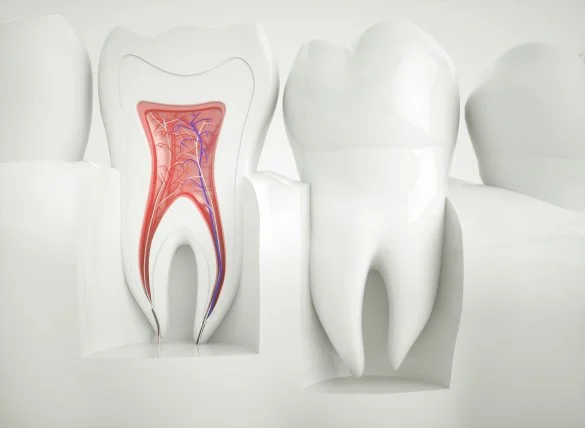

This disease affects the inside of the tooth, also known as the puls. The nerves and vessels within it nourish and sensitize the dental tissue, keeping it alive and healthy. Without it, the unit is considered dead, as nutrients can no longer enter it and supply it with the nutrients it needs. It is a serious disease that should always be treated in time, and which might require root canal in its severe forms.
The infection usually starts affecting the tooth by damaging its enamel. This can be due to lots of causes which cannot be named in their entirety here, but reasons for it usually are:
• Caries: A pathogenic bacterium accumulates on the surface of the tooth, destroying the enamel. Gradually, the infection spreads into the dentin and the pulp becomes infected.
• Trauma: An external injury (a chip or fracture) allows the bacteria to enter, which causes pulpitis in the long run.
Usually three separate treatments lead to pulpitis:
• Caries Treatment: If root canals are not completely sealed, bacteria can accumulate in the cavities under the filling, which causes an infection leading to pulpitis.
• Sanitisation: A procedure to get rid of harmful bacteria in the mouth. If sanitation is not done properly, an infection can develop under the filling or crown.
• Prosthodontics: The dentist grinds the tooth for the crown. The procedure can cause the pulp to overheat (leading to inflammation), which leads to pulpitis.
• Pain in the tooth:: A sharp, stabbing pain appears, especially at night or when touching hot foods. The pain may spread to the jaw.
• An increase in body temperature may occur. This is the immune response to the inflammation in the body.
• The color of the enamel changes. When the pulp is affected, the enamel becomes more opaque and significantly darker.
• These symptoms affect the quality of life: sleep is disturbed by persistent toothache, appetite is lost and headaches may occur.
Inflammation causes severe pain in and around the tooth. At first, the patient can feel the exact location of the inflammation (focal pulpitis), but after a few days, the pain spreads further and the source becomes difficult to understand.
Prolonged pain increases and becomes permanent. Pus builds up inside the tooth, which may either leak through a hole in the enamel or settle in the gum itself. It becomes swollen and painful, and an abscess develops with a fistulous passage (pus escapes through the abscess).
In the case that pulpitis is not treated in a timely manner, advanced pulpitis may turn into a chronic disease. This can be:
• Fibrotic: The vessels carrying blood to the pulp chamber steadily deteriorate. the teeth and enamel stop being nourished and eventually die off. This stage can pass without pain or just with a slight desensitization inside the tooth.
• Gangrene.:Necrosis begins (the pulp dies and rots). May be accompanied by bad breath and darkening of the enamel. It�s usually very easy to spot it when the pulpitis reaches this stage.
• Hypertrophic: An accumulation of soft tissue appears in the root of the tooth. They bleed and interfere with clenching of the jaws
The first time you experience a sharp, throbbing pain, you should seek medical attention immediately, let it be a symptom of pulpitis or not. There are several diagnostic steps that may or may not be performed at the dental clinic during your visit:
• Examination and medical history discussion. It is important to tell the dentist about all your complaints. About when the pain started, if there were reasons for the onset of the disease.
• Percussion: The doctor taps the surface of the tooth, determines the state of the pulp by the sound and feeling of the patient. Different stages of the disease correspond to different responses by the patient.
• Probing: Using a fine probe, the doctor checks the depth of the cavity, the patient's response to pain and the visibility of the pulp.
• Thermodiagnosis: Blowing hot or cold air into the oral cavity to assess tissue response to temperature changes. The patient will be asked of their responses to the changes in heat.
• Electrodiagnosis: Uses an electronic pulse to check nerve sensitivity. The patient is asked for their responses.
• X-rays: Using an x-ray, the doctor observes blackening around the tooth (inflammation). Deep cavities are also a sign of pulpitis. This is usually extremely indicative of whether or not pulpitis exists or not.
The early stages of pulpitis is known as the reversible stage and are treated with easier and less intrusive methods:
• The doctor cleans the cavity. Removes the bacteria that cause the pulp to become inflamed.
• An antibiotic is started. The medication eliminates the inflammation and stops the spread of disease germs.
• A temporary filling is placed over it. After a few days, the doctor opens it. By this time, the infection has cleared up. The doctor then places a permanent filling, which prevents the bacteria from entering the tooth again.
In complicated cases, when pulpitis has advanced and the infection cannot be treated with antibiotics, and the methods mentioned above a root canal surgery is the recommended way to go. We advise you visit Turkey for the treatment, mostly due to advantages of root canal in Turkey. The steps of root canal surgery are:
• If the area is to be left vital, the surgeon removes the living pulp and cleans the cavity. An artificial crown or filling is then placed on the tooth. The pulp is removed completely or partially in one operation, depending on the clinical picture.
• If the area is to be left non-vital, before removing the pulp, the doctor inserts a medication that "kills" the pulp. They then seal the medication with a temporary filling. At the second visit to the clinic (1-2 days later), the doctor removes the pulp, which is already dead and unresponsive, and performs a cleaning and filling of the root canal.
If pulpitis is not treated in time, it may cause the development of other diseases:
• Periodontitis: An infection develops and infects the gums around the inflamed tooth. This causes bleeding, granulomas and cysts which leads to periodontitis.
• Flus: Pus collects in the gum, forming an abscess. The pus then leaks out from under the mucosa, causing a fistula.
• Phlegmon: Occurs due to a complication of a flush. Suppuration spreads, tissue dies, and the disease has no specific location.
• Osteomyelitis: The infection enters the bone tissue of the jaw and begins to destroy it.
• Amyloidosis: Protein metabolism is disrupted due to the constant presence of infection in the body. This can lead to internal organ dysfunction.
• Sepsis: The infection can go deeper into the body and enter the bloodstream. It is difficult to predict how your body will react to this condition. Sepsis can even lead to death in severe cases and thus pulpitis should always be treated in time.